Common Types of Skin Cancer
Skin cancer is typically caused by overexposure to the sun. UV (ultraviolet) rays from the sun have been shown to damage the genetic makeup (or DNA) of cells in laboratory studies. Experts agree this is the reason that sun exposure causes skin cells to genetically mutate into cancer cells. The three main types of skin cancer are:
Basal cell carcinoma
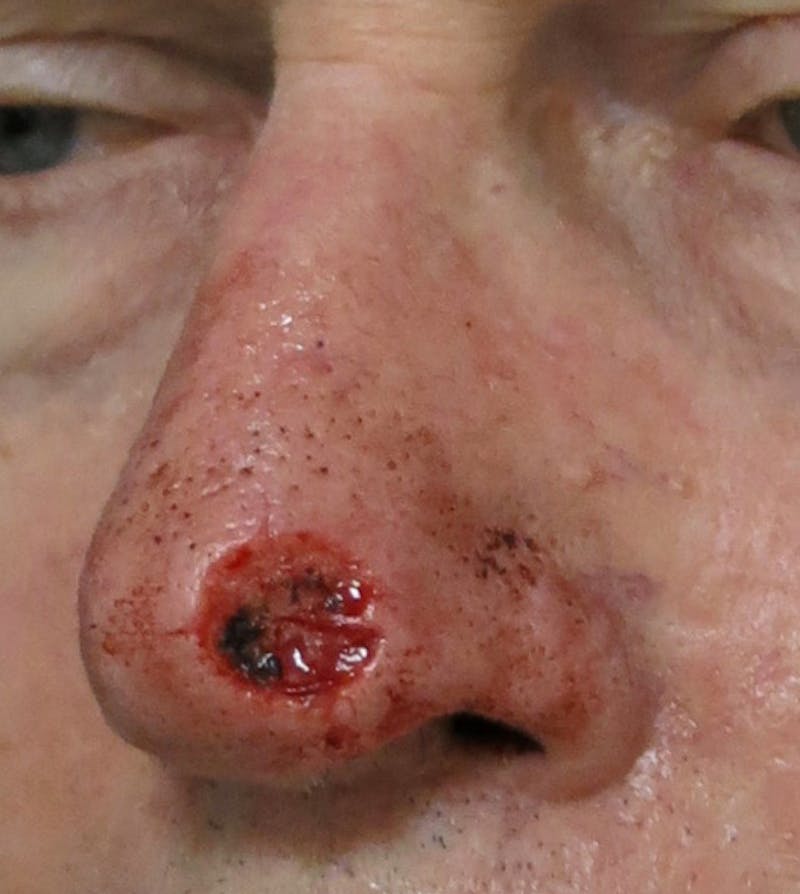
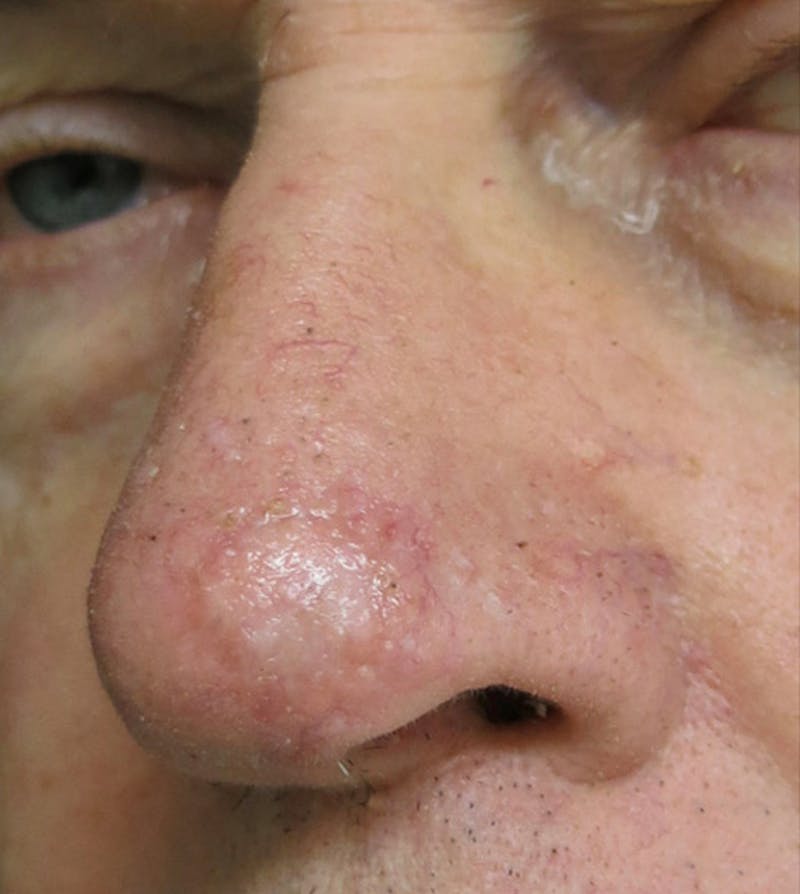
Basal cell carcinoma is the most common and least deadly form of skin cancer. It can, however, be dangerous and grow quickly in its immediate vicinity. It was once commonly referred to as a “Rodent Ulcer” or “Rat Bite Ulcer” due to its ability to eat or gnaw away at nearby tissues as it grows. This can create an expanding sore or ulcer that can be a significant concern, especially on the face when encroaching on important nearby structures such as eyelids, nose, lips, ears, etc.
As this cancer mutates, it may become more and more aggressive, grow faster and cause greater and deeper destruction. With time, this growth may require a much larger surgery to excise it if left untreated. This cancer usually starts to grow slowly on the head, neck, tops of the ears, or anywhere on the upper body. This type of cancer appears in an estimated 75% of skin cancer cases.
Squamous cell carcinoma
Squamous cell carcinoma is responsible for about 20% of skin cancers. It isn’t typically as dangerous as melanoma, but if undiagnosed and left untreated, this type of skin cancer can spread to other parts of the body and become deadly. In general, squamous cell carcinoma is much more dangerous when it appears near any mucous membranes, such as the eyelids, mouth, ear canal, genitals, anus, etc.
Melanoma
Melanoma is considered to be the most dangerous skin cancer. It can become metastatic and spread to other parts of the body such as the brain, liver, lymph nodes, and lung. Although melanoma is responsible for only about 5% of skin cancers, it is responsible for the majority (approximately 75%) of all skin cancer deaths.
Melanoma typically presents as a pigmented lesion or darkly colored spot that changes or varies in color. Staging of melanoma is typically based on the pathology specimen, how deep the tumor has invaded into the skin, if there is any ulceration, or if the cancer has already spread.