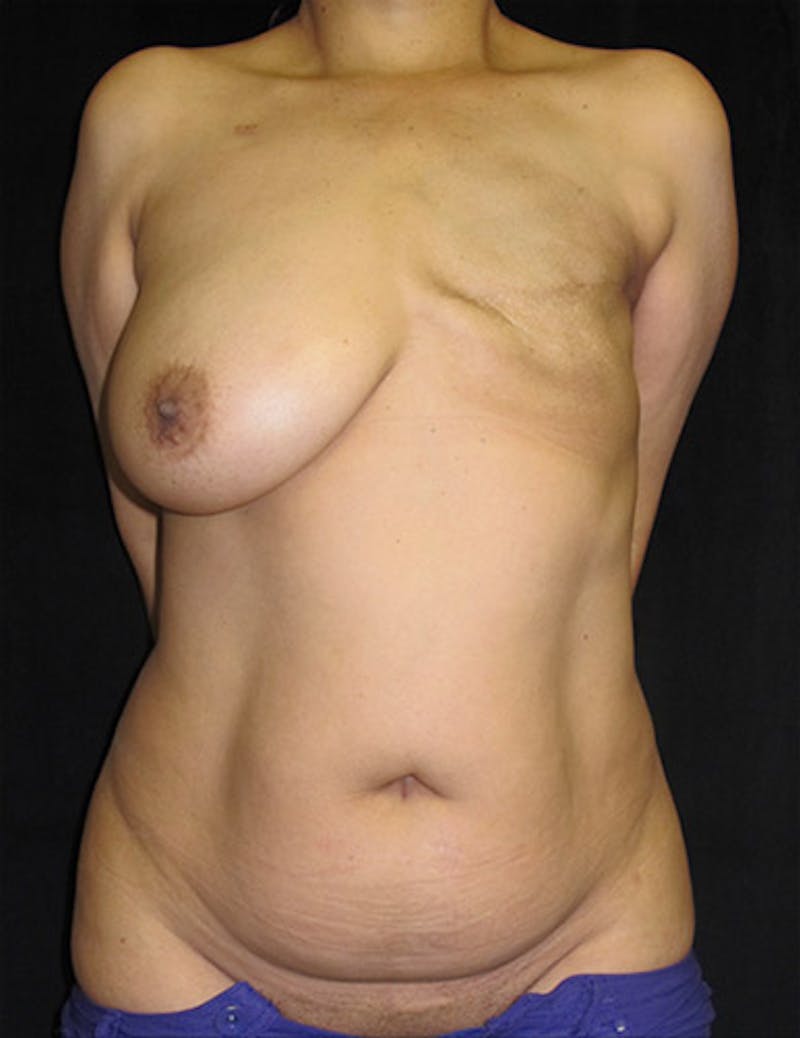
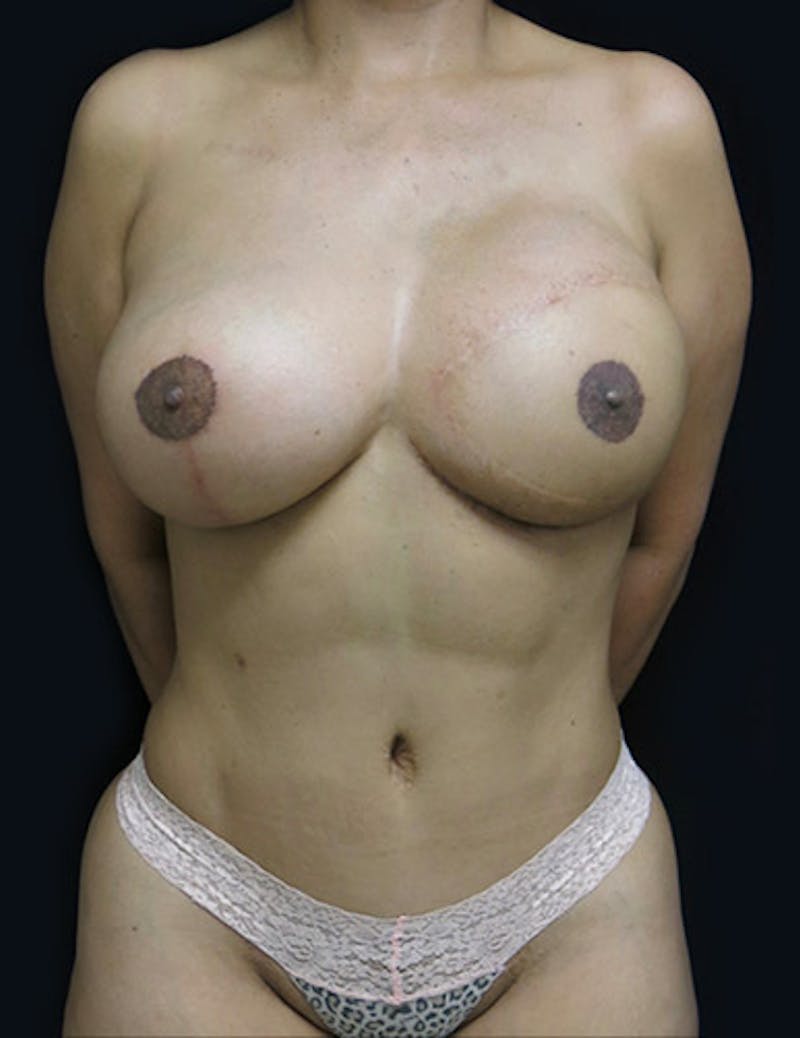
Breast restoration after a mastectomy or lumpectomy is a vital part of the rehabilitation process.
Prophylactic Mastectomy and Breast Reconstruction
Frequently, patients undergo prophylactic mastectomy for genetic reasons. Some patients have a strong family history of breast or ovarian cancer. Genetic testing of these individuals (or their mothers) may reveal a mutation in one of the BRCA genes. BRCA genes normally help protect women from getting breast cancer. However, a mutated BRCA1 gene or BRCA2 gene that does not function correctly is associated with increased genetic damage that may lead to unregulated and rapid cell division. A mutation in one or both of the BRCA genes may be inherited and put the patient at a much higher risk for breast or ovarian cancer in their lifetime. Patients should consider BRCA genetic testing if they have a family history of any of the following:
- Breast cancer diagnosed under the age of 50 years old
- Breast cancer and ovarian cancer
- Both breasts with cancer (bilateral breast cancer)
- Multiple breast cancers
- Males with breast cancer
- Ashkenazi Jewish family descent
- At least two primary types of BRCA1 or BRCA2-related cancers in one family member (pancreatic, fallopian tube, peritoneal, and prostate cancers)
Patients with any concerns or questions regarding breast cancer should seek genetic counseling with a healthcare professional who is experienced in this specialized field. Dr. Lampert can refer you to a qualified healthcare professional for such counseling if there is any question at all.
Patients with a harmful genetic mutation of the BRCA1 or BRCA2 on gene testing may elect to have prophylactic mastectomy performed. Patients having prophylactic mastectomy more frequently are able to have a nipple-sparing mastectomy.